Plantar fasciitis is the leading cause of heel pain worldwide, affecting nearly 10% of the global population. Characterized by a sharp, stabbing pain on the sole of the foot—especially during those first difficult steps in the morning—it is a condition that requires a multidisciplinary approach.
Although it is often dismissed as mere “foot pain,” it is a complex degenerative condition that can significantly impair mobility if left untreated.
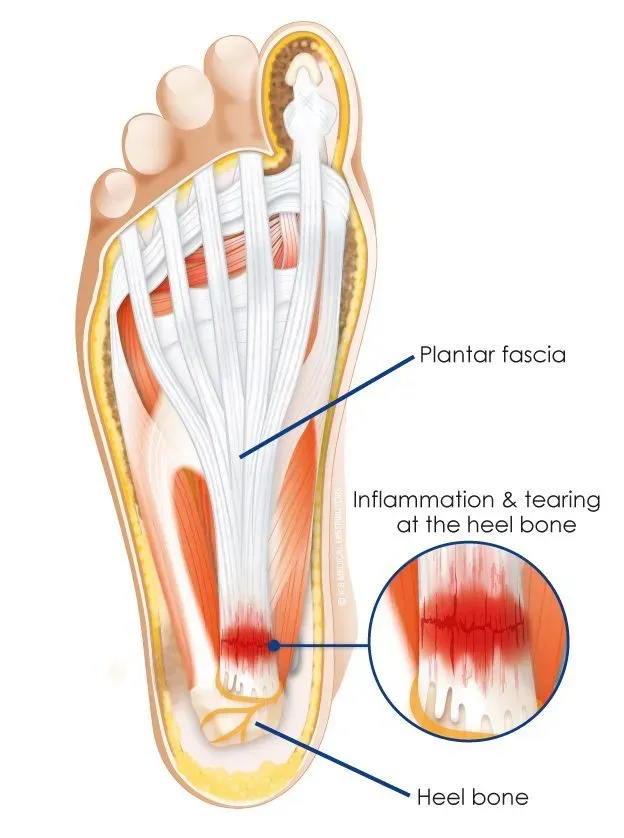
The plantar fascia is a thick band of fibrous tissue that extends from the heel bone to the toes. This band is covered in fat to absorb shock and supports the arch of the foot.
Plantar fasciitis is in most cases unilateral, affecting either the left or right heel. Bilateral plantar fasciitis—that is, affecting both feet simultaneously—is less common, occurring in about one-third of cases.
Based on the latest clinical evidence and expert opinions, this guide explores why this pain occurs and how you can regain your mobility.
Do You Feel Any of These Symptoms?
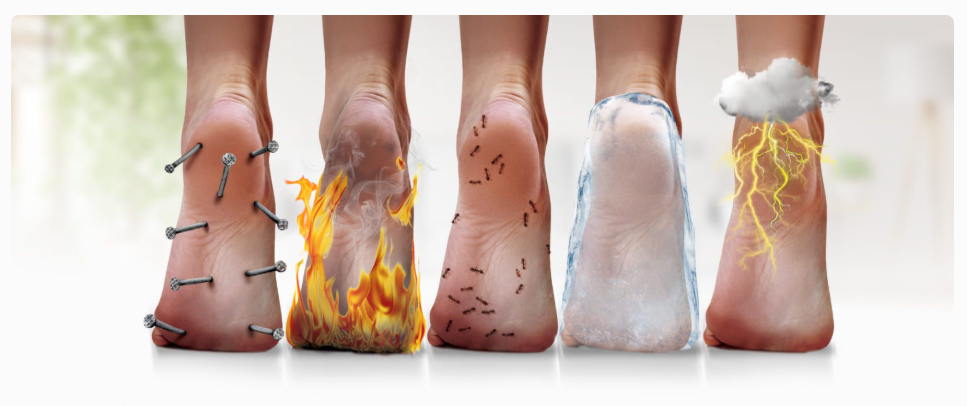
Sharp or shooting foot pain, tingling, numbness, cramping, and soreness—sound familiar? Supportive insoles are essential for daily comfort, providing the support you need to stay on your feet for long hours without pain or discomfort.
Plantar Fasciitis, Sciatica, Heel, Hip or Lower Back Pain and many more… What do all of these ailments have in common? They are all triggered by uncomfortable footwear. When your feet can’t get the right support, your body overcompensates by straining other muscles.
The “First Step” Phenomenon
The hallmark symptom is a stabbing pain near the heel. This pain is typically worst with the first few steps in the morning or after long periods of standing or sitting. Scientifically, this occurs because the fascia tightens and attempts to heal overnight in a shortened position; the first step of the day abruptly re-stretches and re-tears the tissue.
Root Causes and Biomechanical Risk Factors
Understanding why your fascia is failing is the first step toward a permanent cure. Research published in the Journal of Orthopaedic & Sports Physical Therapy identifies several key triggers:
- Age: It is most prevalent between the ages of 40 and 60.
- Biomechanical Factors: Overpronation (flat feet) or an unusually high arch puts excessive strain on the fascia.
- Repetitive Stress: Long-distance running, ballet dancing, and aerobic dance can contribute to early onset.
- Occupational Hazards: Professionals who spend most of their hours on hard surfaces (teachers, factory workers, servers) are at a 3.6x higher risk.
- Obesity: Increased load leads to mechanical collapse of the longitudinal arch.
Regarding the duration of symptoms, it is important to note that ignoring plantar fasciitis in its acute phase can lead to chronic pain.

Can Plantar Fasciitis Be Cured?
The short answer is yes. Clinical data shows that 90% of patients experience significant recovery within the first 8 to 12 weeks of starting a dedicated treatment plan. However, true healing is a marathon, not a sprint; while most see rapid improvement, complete symptom resolution can take up to a year. The key is early intervention—ignoring the initial ‘morning stab’ can lead to chronic degeneration (fasciosis), making professional treatment and proper foot support essential from day one.
What to Avoid: Common Pitfalls
- Walking Barefoot: Especially on hard surfaces like tile or hardwood. This provides zero support and forces the fascia to bear the full weight of the body.
- Ignoring the Pain: Pushing through the pain can turn an acute (temporary) case into plantar fasciosis (chronic degeneration).
- Worn-out Footwear: Shoes that have lost their structural integrity fail to stabilize the calcaneus (heel bone).
Clinical Treatment Pathways
Modern medicine offers a hierarchy of treatments, starting from conservative measures to advanced interventions.
Conservative Gold Standards (90% Success Rate)
- Physiotherapy & Stretching: Focus on the “Gastrocnemius-Soleus” complex (calf muscles). Tight calves are a primary contributor to fascial tension.
- Cryotherapy: Rolling your foot over a frozen water bottle for 15 minutes provides both cold therapy to reduce inflammation and a gentle massage.
- Night Splints: These devices keep the foot in a neutral position overnight, preventing the fascia from shortening.
Plantar Fasciitis Surgery: When is it necessary?
Surgical intervention is considered a last resort, reserved strictly for cases where conservative treatments fail—which happens in only about 5% of patients.
The procedure, known as a plantar fasciotomy, involves releasing 30% to 50% of the fascial fibers to relieve tension. With a success rate between 70% and 80%, results are often enhanced when combined with a gastrocnemius release (calf recession).
Key Indications:
- Chronic Pain: Persistent symptoms lasting more than 9 months.
- Refractory Cases: No response to stretching, orthotics, or shockwave therapy.
Patients can opt for open surgery (ideal if Taris Tunnel Syndrome is present) or endoscopic surgery, which offers the same efficacy with a significantly faster recovery time.
Modern Clinical Treatments – Advanced Non-Invasive Options
Recent clinical trials have shifted the focus from passive rest to active recovery:
- Corticosteroid Injections: Effective for short-term pain relief, though repeated use is discouraged as it may weaken the fascia.
- Extracorporeal Shockwave Therapy (ESWT): A non-invasive procedure that uses sound waves to stimulate healing in the fascial tissue. Studies show a 70% success rate for chronic cases.
- Night Splints: These hold the foot in a dorsiflexed position (toes up) during sleep, preventing the fascia from tightening.
The Role of Nutrition in Recovery
You cannot out-stretch a poor diet. Chronic inflammation in the foot can be exacerbated by systemic inflammation.
- Anti-Inflammatory Superstars: Incorporate Omega-3s (salmon, chia), Curcumin (turmeric with black pepper), and Magnesium to relax muscles.
- Hydration: Proper water intake maintains the elasticity of connective tissues, preventing them from becoming brittle and prone to micro-tears.
Enhancing Quality of Life: Comfort Alternatives
For those looking to improve their comfort without resorting to medical treatments, Akusoli insoles have been gaining popularity. Although they are not a medical “cure,” Akusoli acupressure insoles are specially designed for people who want to lead a more active lifestyle. They help relieve tired, aching feet and completely eliminate pain.

While clinical treatments address the root cause, everyday comfort is vital for managing symptoms.
The Role of Supportive Insoles
Insoles play a crucial role in redistributing pressure away from the heel.
Scientific Insight: A study in Foot & Ankle International found that prefabricated orthotics are often as effective as custom-made ones for the initial management of heel pain.
Featured Option: Akusoli Shoe Insoles
For those seeking a non-clinical comfort boost, Akusoli Shoe Insoles have gained popularity. While they are not a medical “cure,” they offer several features that align with comfort goals:
- Arch Reinforcement: Helps maintain the foot’s natural alignment, reducing the “pull” on the heel.
- Impact Absorption: Targeted cushioning at the calcaneus area to soften the “strike” when walking.
- Magnetic Acupressure: Based on traditional concepts, these zones aim to stimulate blood flow and provide a massage-like sensation, which many users find soothing for foot fatigue.
Most Technologically Advanced
Insoles on the Market
Antimicrobial Silver Coating
Utilizing ion-silver technology to neutralize bacteria on contact, effectively eliminating foot odor and maintaining a sterile environment for skin recovery.
Feet and Arch Support
Dynamic structural engineering that adapts to your unique plantar contours. Provides surgical-grade alignment for flat feet and high arches alike.
Magnetic Technology
Strategically embedded biomagnets create a consistent therapeutic field. This promotes micro-circulation and delivers a passive, restorative massage with every step.
Acupressure Cushions
Precision-mapped zones target high-fatigue areas. By stimulating key reflexology points, it accelerates muscle recovery and reduces the “heavy leg” sensation.
When to See a Specialist
If the pain persists for more than 3–4 weeks despite home care, or if it radiates toward the ankle, consult an orthopedic foot and ankle specialist. A professional evaluation can rule out other conditions like Baxter’s Nerve Neuropathy or stress fractures.
Plantar fasciitis is a marathon, not a sprint. By combining biomechanical correction (insoles and shoes), biological support (nutrition and rest), and physical rehabilitation, most patients can return to a pain-free life within a few months.
Conclusion: A Multi-Pronged Approach
Managing plantar fasciitis requires patience. A combination of stretching the Achilles tendon, using supportive insoles like Akusoli for daily activities, and consulting a specialist for persistent pain is the most effective path to recovery.
Medical Disclaimer & Professional Disclosure
The information provided on this website is for educational and informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Individual results from using Akusoli shoe insoles may vary based on foot morphology and severity of the condition. Always seek the advice of your physician, podiatrist, or other qualified health provider with any questions you may have regarding fasciite plantaire or other chronic foot conditions. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
